Biceps Tendon Rupture
Description
The biceps muscle attaches to the radial tuberosity, which is a small hump on the side of one of the two bones of the forearm (the radius) near the elbow joint. The biceps muscle bends the elbow bringing the hand in toward the body. This muscle also helps to twist the forearm, turning the hand palm up, the motion you use to tighten a screw with a screwdriver. Injury to the biceps usually happens when the arm, bent at the elbow, is forced to straighten. With this injury, the tendon is typically pulled off from its attachment point on the forearm near the elbow joint. This is an unusual injury, affecting only one to two people per 100,000 each year.
The biceps works in conjunction with other muscles that cross the elbow joint. (See Figure 1.) If the biceps tendon ruptures or detaches from the bone, these other muscles make it possible for you to bend the elbow and twist the forearm. However, strength is reduced. Tests have compared the strength of people with a normal healthy arm with those who have injured their biceps tendon. Results show that the injured arm has a loss of 30 percent to 40 percent of its strength, mainly in twisting the forearm.
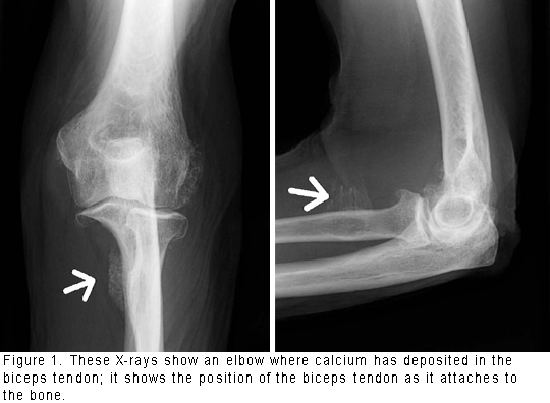
Diagnosis begins by reviewing the events of the injury to determine how the injury occurred. During examination the doctor looks for:
- Swelling in the front of the elbow
- Weakness bending the elbow
- Weakness twisting the forearm against resistance (screwdriver motion)
- Visible bruising
- Gap created by shortening of the biceps tendon on the front of the elbow
X-rays don't usually show biceps tendon rupture abnormalities. They are taken to make sure there are no other problems. Other tests might include ultrasound or an MRI (magnetic resonance imaging) of the elbow to get an image of the disruption.
Risk Factors/Prevention
The usual person with this injury is a male in his 30s to middle-aged. Females very rarely get this injury. The injury is equally likely to occur in the dominant arm or the non-dominant arm. It is usually related to lifting a heavy weight. Smoking and corticosteroid use increase the risk of getting this injury. It is believed that smoking alters nutrition to the tendon. This injury is not usually associated with other medical conditions.
Symptoms
As the tendon disconnects, there is often a feeling or the sound of a pop in the elbow. Some swelling in the front of the elbow is likely. There is weakness when bending the elbow. The biceps muscle and tendon can recoil and shorten, creating a firm swelling in the upper arm and a gap that can often be felt. Following injury, there may not be much pain at rest. Pain is usually felt when using the arm forcefully.
Treatment Options: Non-surgical
Nonsurgical treatment may be considered, especially if there are reasons not to perform surgery and there is less need to restore full strength in the arm. Nonsurgical treatment consists of short-term rest followed by gradually and gently resuming activities. Although other muscles make it possible to bend the elbow fairly well without the biceps, the biceps provides most of the power for turning the forearm. Nonsurgical treatment results in a significant reduction of power (about a 30 percent to 40 percent loss).
Treatment Options: Surgical
Surgical treatment is an appropriate option if a better outcome in terms of strength is required, and surgical risks have been taken into account. The aim of surgical treatment is to return the patient to normal function by reattaching the tendon to the spot where it normally connects.
Timing of surgical treatment is important. Outcome and recovery is improved when you don't delay. Surgery should occur in the first week or two after injury. Scarring of the contracted muscle and tendon can make the surgery more difficult the longer you delay. With long delays it may be impossible to stretch the tendon back to its normal attachment site. The surgery is easier to perform before scar tissue has started to form.
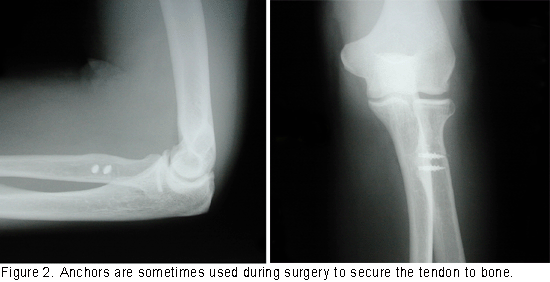
No one method is considered the best overall, so the decision is left to the surgeon. One method involves placing suture material in the tendon to grab it, then attaching the tendon to the bone through drill holes. Another method requires tying the tendon down to manmade devices that are left in place permanently (see Figure 2).
After surgery, one can usually expect to have a very good range of motion and strength nearly equal to the uninjured arm. Long-term difficulties are rare, but it would not be unusual to lose some ability to fully straighten the elbow.
Complications of surgery can include sensory problems in the forearm, which usually go away. Abnormal bone formation might require another operation. At times, abnormal bone can severely limit the twisting motion of the forearm. The overall complication rate is about 9 percent.
The surgeon may recommend physical therapy, splints or slings, depending on the particular case. Physical therapy might help to regain range of motion and strength. Splints or slings might be used for initial rest and for guiding and protecting the injury after motion is resumed. The period of time for complete rest after surgery should not be too long, because some decrease in elbow motion from scarring can occur.
It takes months for the tendon to reform a strong attachment to the bone, so the recovery phase is long. During recovery, vigorous use of the arm, especially for pulling and lifting, should be avoided. A gradual increase in motion and strength training is required.
Activities with the arm are gradually increased, beginning with motion of the elbow while relying on the other hand for power. Another exercise involves light isometric contraction of the biceps muscle without added resistance, and then gradually adding resistance. After a couple of months, more freedom in strengthening can be added. You can return to work with light lifting at this time; however, vigorous use and heavy lifting should be delayed for several months.
January 2006
All Information Copyright © American Academy of Orthopaedic Surgeons
www.aaos.org